Knee Arthritis
Knee Osteoarthritis (Degenerative arthritis of the knee joint)
What is Knee arthritis?
Arthritis means an inflamed painful joint. There are many different types of arthritis (see General Arthritis). The cause of osteoarthritis is multifactorial. The most common type is the degenerative type, this where the articular cartilage (the joint lining) wears away and the underlying bone is exposed, then the two rough surfaces rub together causing pain, limited movement and disability.
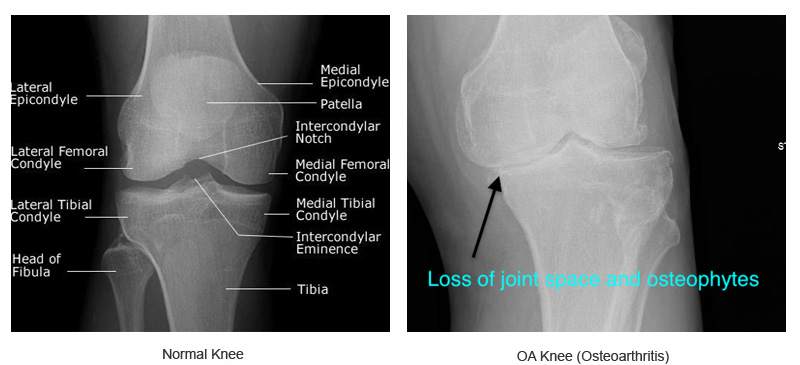
What are the symptoms of Knee arthritis ?
Pain in the knee joint, which can radiate into the shinbone. Swelling and stiffness of the knee joint with restricted movement. Pain may be present at rest, worsen with activity or weight bearing.
There may be difficulty in:
• Walking, putting shoes and socks on, cutting toe nails and getting dressed.
• Getting in and out of the car, climbing stairs and getting in and out of the bath.
• Exercising and playing sport
• Inactivity causing increased stiffness
• Kneeling and squatting
• Overall activity is reduced.
• You may feel the bones rubbing / grating together.
• Sleep being disturbed and morning stiffness.
• Not being able to work.
What investigations are needed?
X rays of the knee joint
Additional investigations may be required in individual cases.
How can it be managed?
Initially conservative measure are utilised to help with the pain and disability which include:
• Activity level and lifestyle can be modified.
• Reducing load on the joint – weight loss.
• Physical therapy and regular non-impact exercise.
• Using a walking stick in the opposite hand.
• Off-loading knee brace
• Simple painkillers, anti–inflammatory medication and supplements can help some patients.
• Knee joint injection with a steroid and local anaesthetic may be of help.
When all these interventions fail a total knee replacement may be an option for you.
You may be suitable for a partial knee replacement if you have knee damage only on one side of the joint. The procedure involves a smaller incision and less bone removal, only one side of your joint is replaced and this can give a shorter hospital stay and more rapid recovery.
What does knee surgery involve?
The knee replacement, replaces both sides of the knee joint and sometimes the knee cap (Patella). It is in essence a resurfacing of the joint. The worn bone surfaces are removed using jigs and cutting blocks to give precise cuts and surfaces to accept the implants and align the knee joint correctly.
Surgery is carried out most commonly under a spinal anaesthetic with sedation.
After surgery you will be monitored and pain controlled.
You will mobilise the same day or certainly the next day with the help of the physiotherapists and progress each day. You will be ready to go home usually day 2 or 3 after surgery and when you feel confident and able to manage at home. Outpatient physiotherapy will be organised for you, and a follow up appointment to see Mr Aslam Mohammed - who will monitor your progress.
What are the risks?
All operations and interventions carry a risk. Measures are taken to reduce some of these risks with early mobilisation, antibiotics, compression stockings and blood thinning medication.
Meticulous surgical technique, attention to detail during your admission and postoperative recovery will aid your recovery.
General risks:
• Anaesthetic
• Cardiac
• Respiratory
• Stroke
Risks specific to the operation:
• Infection – superficial wound and deep joint
• Thrombosis – legs (DVT)
• Pulmonary embolism (PE)
• Leg length difference
• Intraoperative fracture
• Nerve and vessel damage, Complex regional pain syndrome (CRPS)
• Sensitive wounds
• Residual pain and stiffness
• Wearing out of the bearing surface and instability
• Implants becoming loose
• Need for revision surgery
What are the outcomes of knee replacement?
It is generally acknowledged that the results of total knee replacement both functionally and in terms of longevity are very good. The majority of patients have improvement of pain and most patients get back to day-to-day activities. Range of movement and function tend to be improved. However, a proportion (1 in 5) of patients have on-going problems with no obvious cause.
Functional results are maintained over time. With present day materials, bearing surfaces and surgical techniques, there is a 90% chance that your knee replacement will be functioning well at 10 years from the time of being performed and 80% chance of it doing well at 20 years. (See NJR data)
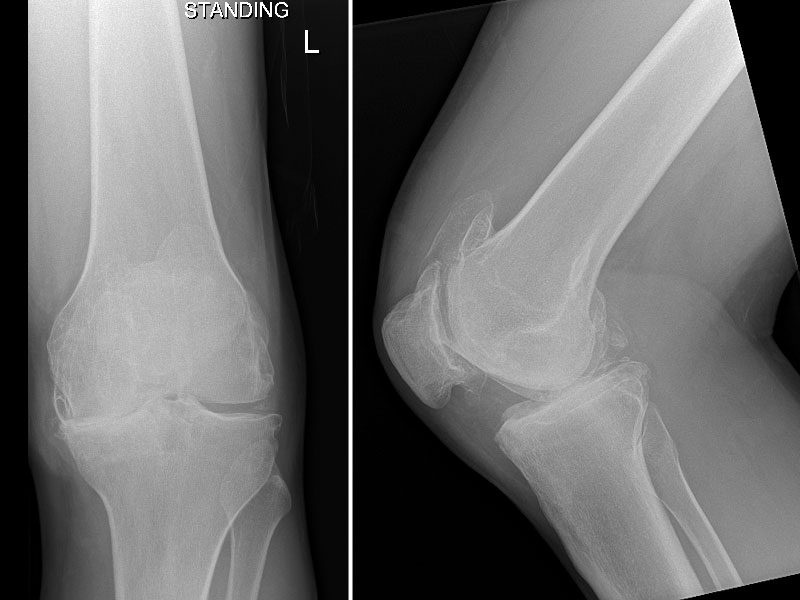 1A. Osteoarthritis of Left knee 48 year old male, he had a total meniscectomy in his teenage years, resulting in arthritis of the knee and bowing of the leg.
1A. Osteoarthritis of Left knee 48 year old male, he had a total meniscectomy in his teenage years, resulting in arthritis of the knee and bowing of the leg.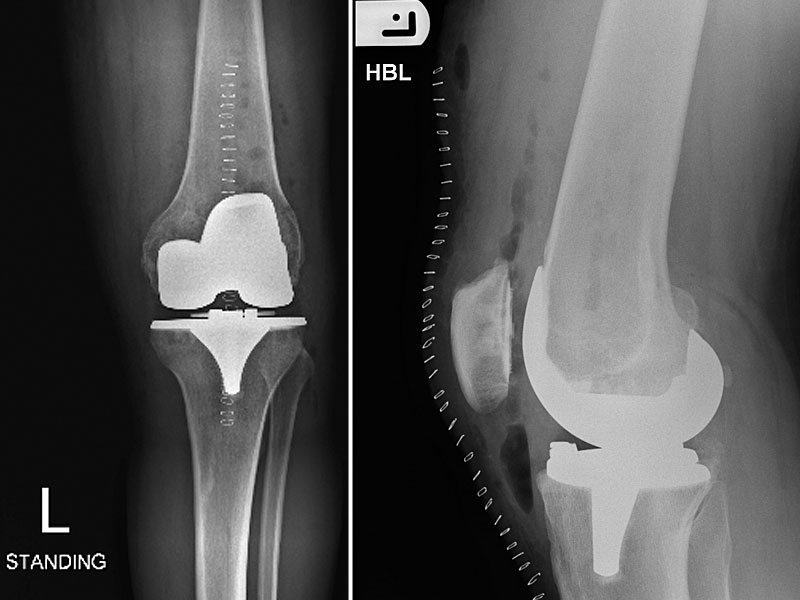
1B. Knee replacement showing the varus deformity (Bowing of the leg) has been corrected and the patella (knee cap) has been resurfaced.
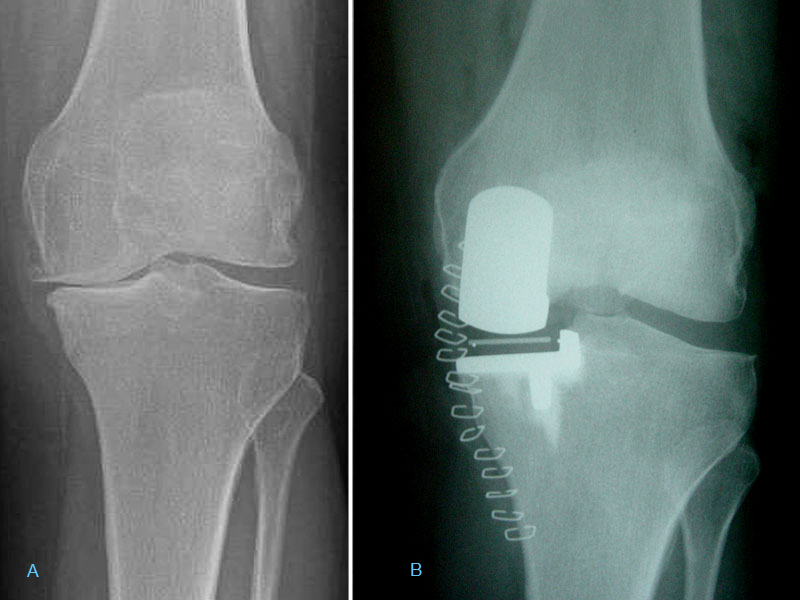 Patient with localised wear on the medial part (inside) of the knee joint, which was suitable for a partial knee replacement. This allows for more natural and better function of the knee joint.
Patient with localised wear on the medial part (inside) of the knee joint, which was suitable for a partial knee replacement. This allows for more natural and better function of the knee joint.
2A. Knee showing medial OA
- Arthritis
- Knee Arthritis
- Knee Replacement
- Knee Sports Injury
- Knee Arthroscopy
- Knee Meniscus Tears
- Anterior Cruciate Ligament
- Chondral Injury / Cartilage Injury
North West Hip & Knee Clinics
Services provided:
• Keyhole (minimally invasive)
• Hip and Knee Surgery
• Hip and Knee Joint Replacement
• Hip and Knee Sports Injury
• Hip Arthroscopy, FAI and Labral Surgery
• Knee Arthroscopy - Meniscus surgery
• Knee Arthroscopy and ACL / PCL
• Ligament Reconstruction
• Biologics – PRP, Stem Cell
• Cartilage Regeneration
Mr Aslam Mohammed Consultant Hip and Knee Surgeon